- Bone Health
- Brain Health
- Fitness
- Gastrointestinal
- Hair
- Healthy Aging
- Heart Health
- Hot Flashes
- Joint and Muscle Aches
- Menopause
- Mental Health
- Mindfulness
- Mood Swings
- Nutrition
- Pelvic Floor
- Products
- Relationships
- Sexual Wellness
- Skin
- Sleep
- Urogenital
- Weight Management
Blog Archive

Revolutionizing Workplace Inclusivity: New Research on Menopause and Work
New study by SRI International and Lisa Health uncovers challenges faced by menopausal women in the workplace.

Product Review: Radical Skincare
Radical Skincare offers women advanced natural skincare solutions for aging skin.

Measuring Perimenopause Hormone Levels
Perimenopause hormone testing is not as straightforward as it may seem.

PCOS and Menopause
Polycystic ovary syndrome (PCOS) is about more than irregular periods. As you approach menopause, learn how PCOS can affect your health.

How to Balance Exercise and Intermittent Fasting
Food is critical for fueling and recovering from exercise. If you’re intermittent fasting, here’s how to make sure your workouts help your body get stronger—not more stressed.
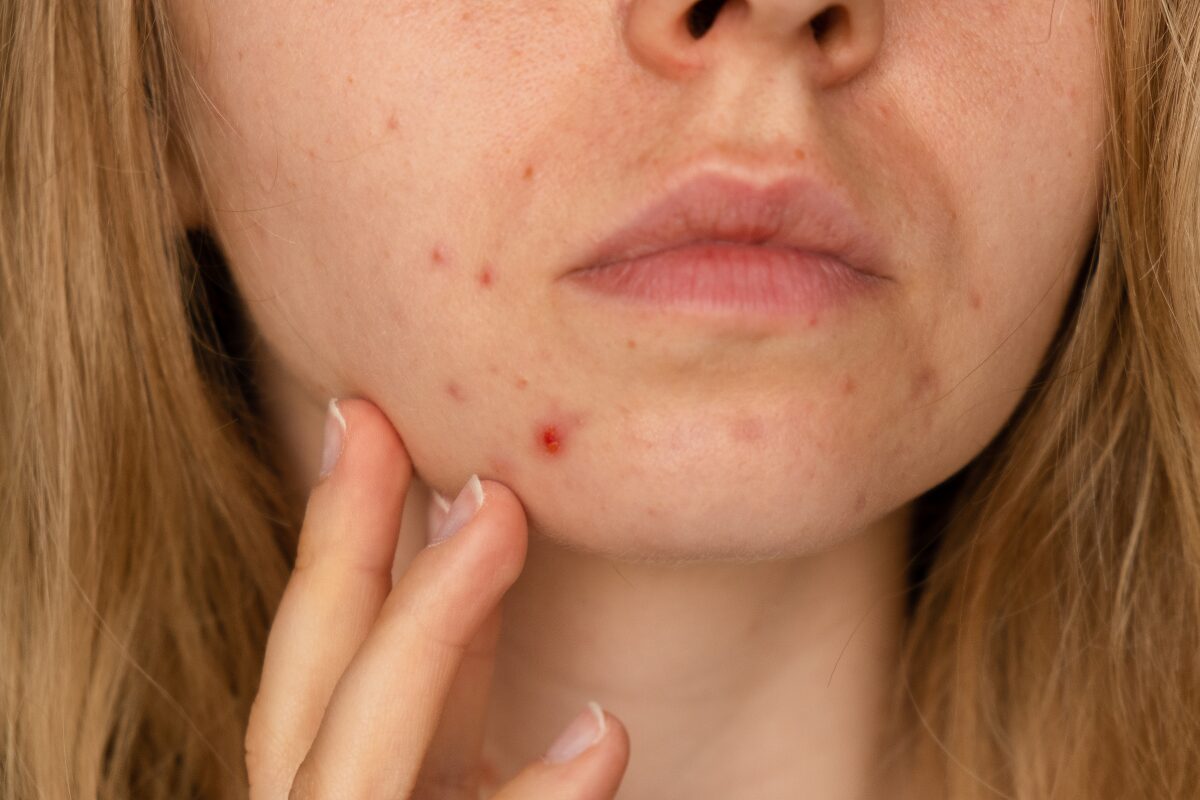
Menopausal Acne: How to Deal With Midlife Breakouts
Hormonal changes often lead to breakouts. Here’s how to manage menopausal acne.

Menopause Health Trends We’re Watching in 2024
Here’s a quick look at seven trends that we’ll be watching in 2024.